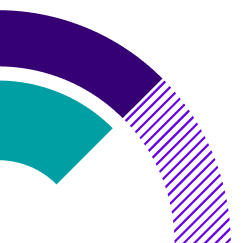
Eliminate manual tasks and automatically identify opportunities for earlier discharge, all without leaving the EHR.
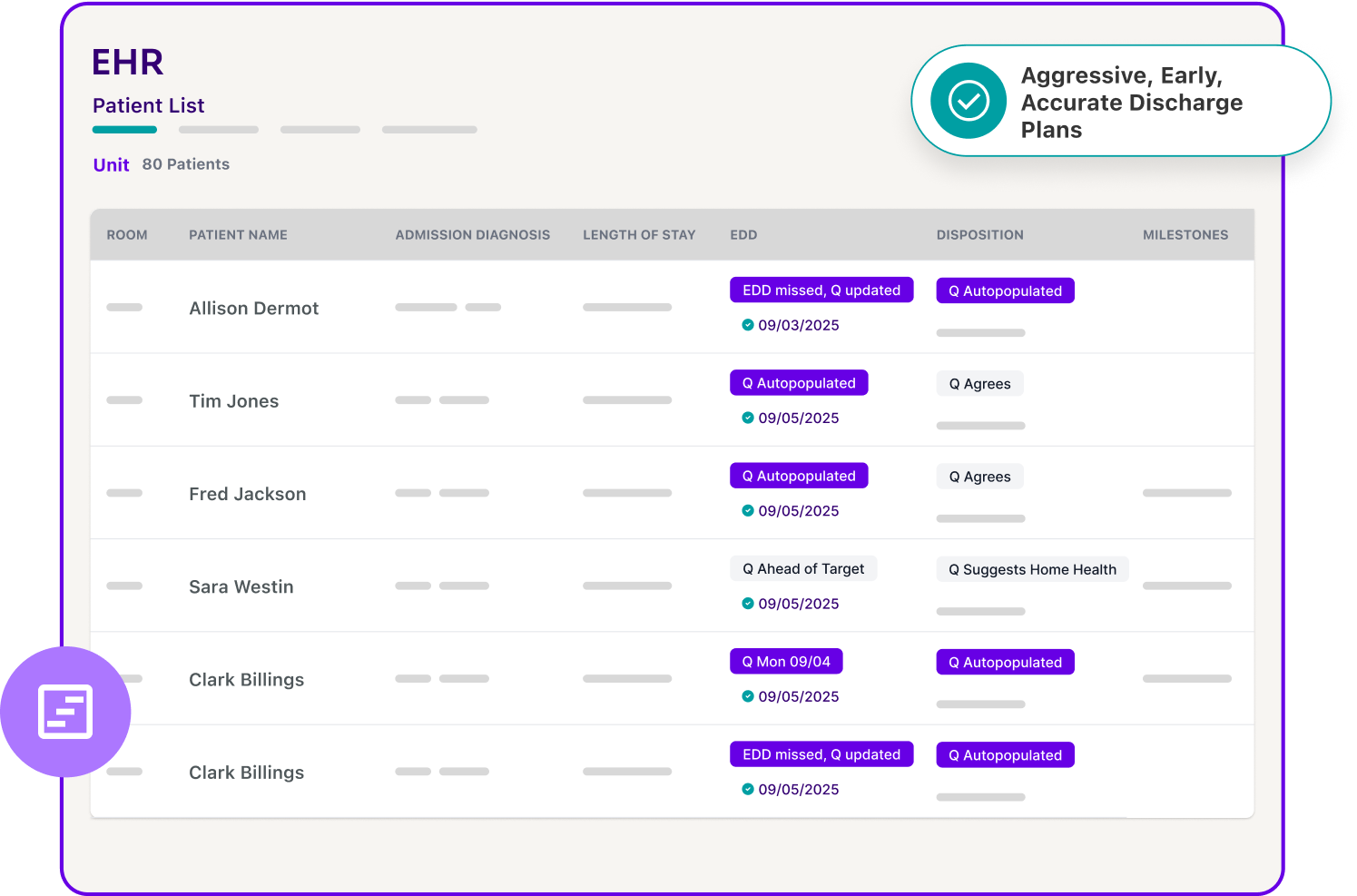
Machine learning models—locally trained on your patients and care patterns—auto-populate EDD and dispositions directly into the EHR on the first morning after admission.
Get patients to their next most appropriate site of care sooner
Enable early team alignment
Keep discharge plans up to date automatically
Lower administrative burden
Using a sophisticated algorithm, including multiple machine learning models, our solution automatically sequences ancillary orders to best support patient flow and discharge success. This increases high priority order completion by 15-25%, yielding .27 and .49 days savings, respectively, for Echo and MRI orders.
The faster patients can get through therapy, imaging, and lab services, the sooner a bed opens up for a new patient.
Eliminate back and forth between teams
Reduce manual sequencing steps
Factor in facility-specific resources
Ensure optimal patient flow
Our library of care gap orchestrations evaluates each patient care plan to identify and resolve gaps that could delay discharge, such as physical therapy, MRI, case management consults, foleys, and more.
Predict discharge barriers for the whole care team
Set milestones in an optimal order
Proactively unblock at-risk care flows
Avoid delays & last-minute scrambles
Optimize post-acute patient placement
Accelerate patient throughput
Reduce SNF over-utilization
Minimize risk of excess days
Reduce delays and enhance discharge efficiency for better patient care
Easily identify and deploy the right staff
Ensure discharge success
Allocate resources effectively based on up-to-the-minute patient data

Accelerate ROI on new technology
Deliver intelligence right in teams’ workflows
Reduce care team burden
See, know, act, all on a single screen
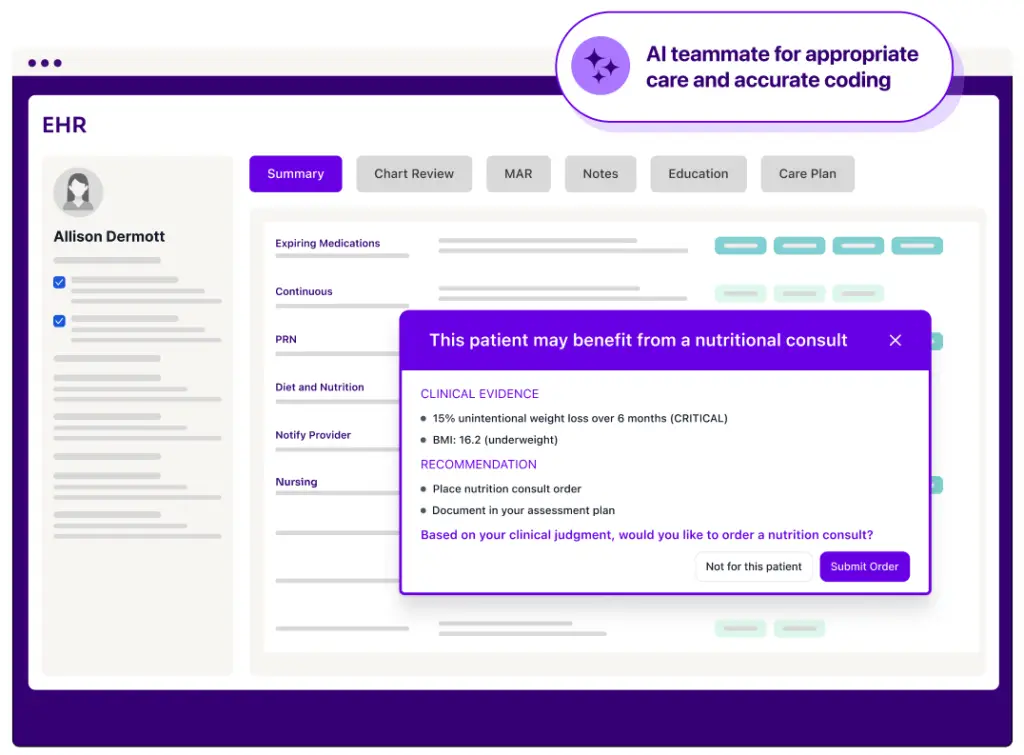
Surface malnutrition risk to drive timely care and accurate documentation, shortening length of stay by 2 days, reducing readmissions by 27%, and adding $10k in reimbursement per patient