Today, frontline teams are more burned out than ever: clinical staff turnover has accelerated, with many deciding to exit the workforce altogether. At the same time, health systems have never been in a more precarious position: length of stay has risen significantly, which compresses margins, constrains bed capacity, and ties up existing staff. Fortunately, recent research shows that early discharge planning can significantly reduce length of stay. But how can health systems empower care teams to put this in practice — without adding to an already crushing workload?
Highly Effective Multidisciplinary Discharge Rounds (MDRs):
The Cornerstone to Early Discharge Planning
Qventus has worked with hundreds of units across large health systems, community hospitals, and academic medical centers to hardwire early discharge planning. Through this experience, we have established Highly Effective MDRs that combine process and technology changes to help care teams maximize MDRs for discharge planning.
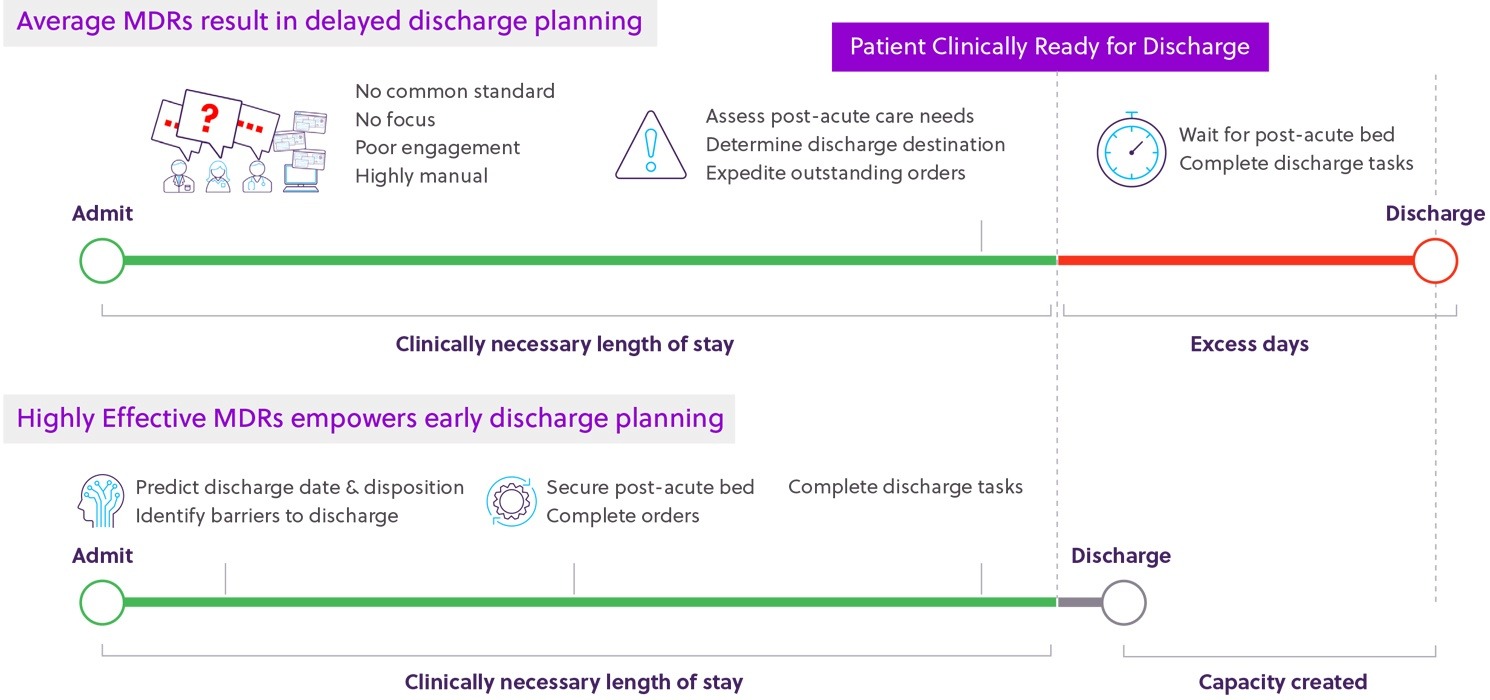
While many hospitals have attempted to implement MDRs, the average MDR today has no common standard, lacks focus, and suffers from poor engagement. In contrast, Highly Effective MDRs engage teams in aligning on discharge goals and key activities needed to achieve them, effectively using technology such as AI and automation to reduce low value-added, manual work. Through this approach, care teams can anticipate issues with enough lead time to resolve them and keep the discharge plan up to date as conditions evolve. This allows organizations to reduce length of stay, improve care experience, and decrease workload intensity.
5 Best Practices for Highly Effective MDRs
Qventus emphasizes 5 key strategies for implementing Highly Effective MDRs:
- Make MDRs a strategic priority: Leaders need to take the right strategic steps to build a coalition of champions, articulate the benefits of MDRs, and implement a standard MDR structure.
- Convene the right team in the right roles: Having the right disciplines represented with clearly defined roles ensures consistency, ownership, and efficiency
- Focus the conversation on the discharge plan: Research shows that aligning on key components of the discharge plan early in the stay can drive significant impact
- Use technology to make MDRs & follow-up easier: AI and automation can empower teams to improve planning quality, reduce manual steps, decrease clicks
- Leverage data to drive and sustain best practices: Without ongoing reinforcement, engagement begins to wane as soon as ~4 weeks after initial implementation
Together, these best practices enable hospitals to create a culture that emphasizes MDRs and early discharge planning across the organization.
Learn More
Read our new ebook to learn more about how to implement Highly Effective MDRs to help your teams drive early discharge planning, deliver a better care experience, and reduce length of stay — while decreasing workload intensity.


